The parasympathetic nervous system plays a vital role in regulating the functions of the gut. Understanding its mechanisms and the impact it has on gastrointestinal health is crucial for both healthcare professionals and individuals seeking to optimize gut function. In this comprehensive overview, we will delve into the intricate relationship between the parasympathetic nervous system and the gut, exploring its role, components, and potential dysfunctions. Please note that while this article aims to provide valuable insights, it is important to consult with a healthcare professional for personalized advice and guidance.
Understanding the Parasympathetic Nervous System
The parasympathetic nervous system is one of the two divisions of the autonomic nervous system, working in tandem with the sympathetic nervous system to maintain homeostasis. Often referred to as the “rest and digest” system, the parasympathetic nervous system counterbalances the fight-or-flight response triggered by the sympathetic division. It conserves energy and promotes processes that aid digestion, assimilation, and overall gut function.
When it comes to the intricate workings of the human body, the parasympathetic nervous system plays a vital role in maintaining our overall well-being. It is responsible for a multitude of functions that are essential for our survival and daily functioning.
The Role of the Parasympathetic Nervous System
In the gut, the parasympathetic nervous system regulates a wide range of functions, including the secretion of digestive enzymes, motility, blood flow, and nutrient absorption. It stimulates the production of saliva, gastric acid, and pancreatic enzymes, all crucial for efficient digestion. Additionally, it supports the relaxation of sphincter muscles, allowing for the smooth passage of food through the gastrointestinal tract.
Imagine a well-orchestrated symphony, where each instrument plays its part to create a harmonious melody. Similarly, the parasympathetic nervous system orchestrates the intricate dance of digestion, ensuring that each step is executed with precision and efficiency.
Key Components of the Parasympathetic Nervous System
The parasympathetic nervous system can be divided into two main components: the cranial and the sacral divisions.
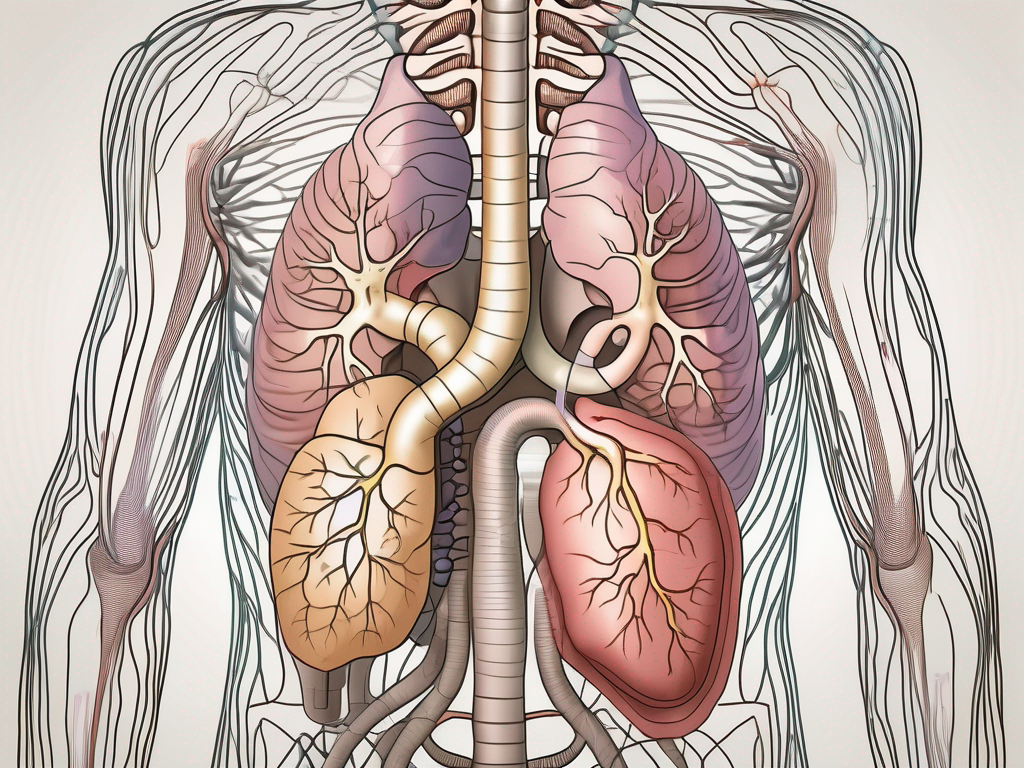
The cranial division of the parasympathetic nervous system originates from the cranial nerves, specifically the oculomotor nerve (III), facial nerve (VII), glossopharyngeal nerve (IX), and vagus nerve (X). These nerves innervate various organs and structures, including the eyes, salivary glands, heart, lungs, liver, stomach, and intestines. They ensure that these organs receive the appropriate signals to carry out their functions optimally.
On the other hand, the sacral division of the parasympathetic nervous system arises from the sacral spinal cord segments (S2-S4). It innervates the pelvic organs, such as the bladder, reproductive organs, and lower gastrointestinal tract. Through its intricate network of nerves, the sacral division ensures the proper functioning of these vital organs, contributing to our overall well-being.
Together, the cranial and sacral divisions of the parasympathetic nervous system work in harmony, creating a symphony of bodily functions that allow us to thrive and lead healthy lives.
The Gut and Its Nervous Supply
The gut, or gastrointestinal tract, is a complex system responsible for the digestion and absorption of nutrients. It extends from the mouth to the anus, encompassing various organs, including the esophagus, stomach, small intestine, and large intestine.
The process of digestion begins in the mouth, where food is broken down by chewing and mixed with saliva. From there, the food travels down the esophagus, a muscular tube that connects the mouth to the stomach. The esophagus uses rhythmic contractions, called peristalsis, to push the food towards the stomach.
Anatomy of the Gut
The gut is a highly organized structure, consisting of layers of smooth muscle, nerves, blood vessels, and specialized cells responsible for digestion and absorption. Its anatomical complexity supports efficient digestion and ensures the continuous movement of food throughout the digestive system.
The stomach, located in the upper abdomen, is a muscular organ that further breaks down food through the secretion of gastric juices. These juices contain enzymes and acids that help to break down proteins and kill bacteria. The stomach also serves as a temporary storage site for food before it moves into the small intestine.
The small intestine is a long, coiled tube that is divided into three parts: the duodenum, jejunum, and ileum. It is in the small intestine that most of the digestion and absorption of nutrients takes place. The inner lining of the small intestine is covered in finger-like projections called villi, which increase the surface area for absorption.
After the small intestine, the partially digested food enters the large intestine, also known as the colon. The colon absorbs water and electrolytes from the remaining undigested material, forming solid waste products. The waste products are then stored in the rectum until they are eliminated from the body through the anus.
The Enteric Nervous System: The Gut’s Own Brain
Within the gut, there exists a complex network of nerves called the enteric nervous system (ENS). Often referred to as the “second brain,” the ENS is composed of millions of neurons that coordinate gut motility, regulate secretions, and communicate with the central nervous system. It acts independently but also interacts with the parasympathetic and sympathetic divisions.
The enteric nervous system plays a crucial role in the regulation of digestion. It receives sensory information from the gut and responds by coordinating the contraction and relaxation of the smooth muscles in the digestive tract. This allows for the smooth movement of food through the gut, ensuring efficient digestion and absorption of nutrients.
In addition to its role in digestion, the enteric nervous system also communicates with the central nervous system, which includes the brain and spinal cord. This bidirectional communication allows for the integration of gut functions with other bodily processes, such as appetite regulation, stress response, and immune function.
Furthermore, the enteric nervous system contains a variety of neurotransmitters, including serotonin, dopamine, and gamma-aminobutyric acid (GABA). These neurotransmitters not only regulate gut motility but also play a role in mood regulation and overall well-being.
In conclusion, the gut and its nervous supply are intricately connected, working together to ensure the proper digestion and absorption of nutrients. The enteric nervous system acts as the gut’s own brain, coordinating gut motility and communicating with the central nervous system. Understanding the anatomy and function of the gut is essential for maintaining a healthy digestive system and overall well-being.
The Parasympathetic Nerve Supply to the Gut
The parasympathetic nervous system supplies the gut through two primary pathways: the vagus nerve and the sacral parasympathetic nerves.
The parasympathetic nervous system, often referred to as the “rest and digest” system, plays a crucial role in regulating various bodily functions, including digestion. It works in opposition to the sympathetic nervous system, which is responsible for the “fight or flight” response.
The Vagus Nerve: A Critical Connection
The vagus nerve, also known as the tenth cranial nerve, is responsible for transmitting parasympathetic signals from the brain to the gut. It is the primary pathway for the parasympathetic control of the upper digestive tract.
Originating from the medulla oblongata in the brainstem, the vagus nerve extends down through the neck, thorax, and abdomen, branching out to innervate various organs along the way. Its extensive reach allows it to exert control over a wide range of digestive processes.
One of the key functions of the vagus nerve is the regulation of gastric acid secretion. It stimulates the release of acetylcholine, a neurotransmitter that activates the production of gastric acid in the stomach. This acid is essential for the breakdown of food and the absorption of nutrients.
In addition to acid secretion, the vagus nerve also influences gastric motility. It stimulates the contraction of the smooth muscles in the stomach, helping to propel food through the digestive system. This coordinated movement ensures that food is properly mixed with digestive enzymes and thoroughly broken down before entering the small intestine.
Furthermore, the vagus nerve plays a role in the regulation of other essential digestive processes, such as pancreatic enzyme secretion and bile production. By stimulating the pancreas and the liver, it ensures that the necessary enzymes and bile are released into the small intestine to aid in the digestion and absorption of fats, proteins, and carbohydrates.
The Sacral Parasympathetic Nerves
Alongside the vagus nerve, the sacral parasympathetic nerves contribute to the parasympathetic innervation of the gut. Originating from the sacral region of the spinal cord, these nerves innervate the lower part of the digestive tract, including the colon and rectum.
The sacral parasympathetic nerves play a crucial role in regulating the functions of the lower digestive tract. They control the motility of the colon, ensuring the smooth movement of waste materials towards the rectum for elimination.
In addition to motility, the sacral parasympathetic nerves also influence the sensation and perception of rectal fullness. When the rectum becomes distended with feces, these nerves send signals to the brain, triggering the urge to defecate.
Furthermore, the sacral parasympathetic nerves are involved in the regulation of the internal anal sphincter. This sphincter, composed of smooth muscle, helps to maintain continence by keeping the anus closed. The parasympathetic signals from the sacral nerves relax the internal anal sphincter, allowing for the passage of feces during defecation.
In summary, the parasympathetic nerve supply to the gut is a complex network that involves both the vagus nerve and the sacral parasympathetic nerves. These pathways work together to regulate various digestive processes, ensuring the efficient breakdown and absorption of nutrients. Understanding the intricate connections between the nervous system and the gut is crucial for maintaining optimal digestive health.
Functions of the Parasympathetic Nerve in the Gut
The parasympathetic nerve plays a crucial role in maintaining the optimal functioning of the gut. It exerts its influence over various aspects of gut function, ensuring the efficient digestion and absorption of nutrients.
Digestion and the Parasympathetic Nerve
When the parasympathetic nervous system is activated, it sets in motion a series of events that are vital for effective digestion. One of its primary functions is to stimulate the release of saliva, which contains essential digestive enzymes. These enzymes, such as amylase, lipase, and protease, play a crucial role in breaking down complex carbohydrates, fats, and proteins, respectively. The parasympathetic nerve ensures that the mouth produces an adequate amount of saliva to initiate the breakdown of food as soon as it enters the oral cavity.
Furthermore, the parasympathetic nervous system promotes the production of gastric acid in the stomach. This acid is essential for the breakdown of proteins into smaller peptides and amino acids. It also creates an acidic environment that helps activate various digestive enzymes, such as pepsin, which further aids in the digestion of proteins. The parasympathetic nerve ensures that the stomach secretes an optimal amount of gastric acid, facilitating the breakdown of proteins and aiding in the absorption of key nutrients.
The Parasympathetic Nerve and Gut Motility
In addition to its role in digestion, the parasympathetic nervous system also plays a crucial role in regulating gut motility. It stimulates the contraction of smooth muscles within the gastrointestinal tract, allowing for the synchronized movement of food along the digestive system. This coordinated peristaltic activity ensures proper mixing, propulsion, and absorption of nutrients.
When the parasympathetic nerve is activated, it triggers a series of muscle contractions that propel food through the esophagus and into the stomach. From there, it continues to stimulate the rhythmic contractions of the stomach muscles, known as gastric peristalsis. These contractions help break down the food into smaller particles and mix it with gastric acid and digestive enzymes.
As the food moves into the small intestine, the parasympathetic nerve continues to exert its influence. It stimulates the contraction of the smooth muscles in the intestinal walls, promoting the movement of food along the small intestine. This movement allows for the thorough mixing of food with digestive enzymes and facilitates the absorption of nutrients into the bloodstream.
Furthermore, the parasympathetic nerve also plays a role in regulating the movement of food through the large intestine. It stimulates the contractions of the colon muscles, aiding in the formation and elimination of feces.
In summary, the parasympathetic nerve is responsible for coordinating various aspects of gut function. From the initial release of saliva and gastric acid to the rhythmic contractions of the stomach and intestines, it ensures that the digestive process runs smoothly. By understanding the functions of the parasympathetic nerve in the gut, we can appreciate the intricate mechanisms that allow our bodies to efficiently digest and absorb the nutrients we need for optimal health.
Disorders Related to Parasympathetic Nerve Dysfunction in the Gut
Parasympathetic nerve dysfunction can lead to several gastrointestinal disorders, impacting overall gut health and quality of life. The parasympathetic nervous system plays a crucial role in regulating various bodily functions, including digestion and gut motility.
When the parasympathetic nerves in the gut are not functioning properly, it can result in the development of disorders such as irritable bowel syndrome (IBS) and gastroparesis. These conditions can cause a range of symptoms that can significantly affect an individual’s daily life.
Irritable Bowel Syndrome and Parasympathetic Nerve Dysfunction
Irritable bowel syndrome (IBS) is a common gastrointestinal disorder characterized by symptoms such as abdominal pain, bloating, and irregular bowel habits. It is a chronic condition that can have a significant impact on a person’s quality of life.
Research suggests that alterations in parasympathetic nerve activity may contribute to the development and exacerbation of IBS symptoms. The parasympathetic nervous system plays a vital role in regulating gut motility, secretion, and blood flow. Dysfunction in this system can disrupt the normal functioning of the gut, leading to the characteristic symptoms of IBS.
However, further studies are needed to fully elucidate the relationship between IBS and parasympathetic dysfunction. Understanding the underlying mechanisms can help in the development of targeted therapies for managing IBS symptoms and improving the overall well-being of affected individuals.
Gastroparesis: A Result of Vagus Nerve Damage
Gastroparesis is a condition characterized by delayed gastric emptying due to impaired or damaged vagus nerve function. The vagus nerve, a major component of the parasympathetic nervous system, controls the movement of food from the stomach to the small intestine.
When the vagus nerve is damaged or not functioning properly, the stomach’s ability to contract and empty its contents is compromised. This can lead to symptoms such as early satiety, nausea, vomiting, and bloating. The delayed gastric emptying can also result in poor nutrient absorption and fluctuations in blood sugar levels.
Management of gastroparesis often involves dietary modifications, medications, and other therapeutic interventions. Dietary changes may include consuming smaller, more frequent meals and avoiding foods that are difficult to digest. Medications can help stimulate stomach contractions or manage symptoms such as nausea and vomiting. In severe cases, surgical interventions may be necessary to improve gastric emptying.
Research into the underlying causes and potential treatments for gastroparesis is ongoing. By understanding the role of parasympathetic nerve dysfunction in the development of this condition, healthcare professionals can develop more effective strategies for managing symptoms and improving the quality of life for individuals with gastroparesis.
Therapeutic Approaches for Parasympathetic Nerve Dysfunction
When parasympathetic nerve dysfunction affects gut health, various therapeutic approaches can help manage symptoms and improve overall well-being.
Medications for Parasympathetic Nerve Disorders
Depending on the specific diagnosis, healthcare professionals may prescribe medications to modulate parasympathetic activity and alleviate symptoms. These medications can target specific receptors or enzymatic processes involved in parasympathetic signaling.
Surgical Interventions and the Parasympathetic Nerve
In severe cases of parasympathetic nerve dysfunction, surgical interventions may be necessary. Procedures such as vagotomy, which involves cutting or removing sections of the vagus nerve, can be considered as a last resort option. However, extensive research and evaluation are essential before pursuing surgical interventions.
Future Directions in Parasympathetic Nerve Research
Advancements in the understanding of the parasympathetic nervous system and its role in gut health are constantly emerging. As researchers delve deeper into this complex field, new therapeutic modalities and approaches are being explored.
Emerging Therapies for Parasympathetic Nerve Disorders
Ongoing research is shedding light on novel therapeutic options for parasympathetic nerve disorders. From targeted drug therapies to innovative neuromodulation techniques, these emerging therapies show promise in restoring parasympathetic balance and improving gut function.
The Future of Gut-Brain Axis Research
The gut-brain axis, a bidirectional communication system between the gut and the central nervous system, is a rapidly evolving area of research. Further investigations into the intricate interplay between the parasympathetic nervous system, the enteric nervous system, and the gut microenvironment may unlock new insights into gut health and pave the way for innovative treatment modalities.
Conclusion
Understanding the parasympathetic nerve’s role in supplying and regulating the gut is instrumental in comprehending gastrointestinal health. From its intricate anatomy and communication pathways to its impact on digestion and its potential dysfunctions, the parasympathetic nervous system plays a pivotal role in maintaining optimal gut function. Consulting with a healthcare professional can help identify and manage any parasympathetic nerve-related disorders, ensuring the best possible outcomes for gut health and overall well-being.